Laproscopy& Hysteroscopy
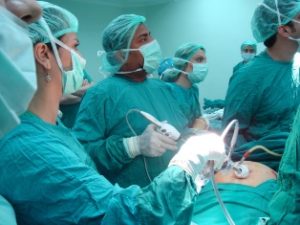
Laparoscopy is a surgical procedure that involves the insertion of a narrow telescope-like instrument through a small incision in the belly button. This allows visualization of the abdominal and pelvic organs including the area of the uterus, the fallopian tubes, and ovaries.
This procedure allows us to determine whether there are any defects such as scar tissue, endometriosis, fibroid tumors and other abnormalities of the uterus, fallopian tubes, and ovaries.
If any defects are found then they can sometimes be corrected with operative laparoscopy which involves placing instruments through ports in the scope and through additional, narrow (5 mm) ports which are usually inserted at the top of the pubic hairline in the lower abdomen.
Because of the cost and invasive nature of laparoscopy, it should not be the first test in the couples diagnostic evaluation. In general, semen analysis, hysterosalpingogram, assessment of ovarian reserve and documentation of ovulation should be assessed prior to consideration of laparoscopy. For example, if the woman has a clear ovulation problem or her male partner has a severe sperm defect then it is unlikely that laparoscopy will provide additional useful information that will help them conceive.
Laparoscopy was part of the standard female infertility work-up until the mid-1990s. Before then most reproductive endocrinology and infertility specialists did laparoscopy prior to using gonadotropins for superovulation of the ovaries as a fertility treatment. However, this tradition has been challenged as being of questionable benefit when assessed by its cost-effectiveness and invasiveness.
Fertility clinics are doing far less diagnostic laparoscopy today than in the 1980s and 1990s. Much of this is due to the major advances in IVF technologies and the resulting increases in IVF success rates. Couples are carefully considering the costs of fertility treatments for women. They are asking for insemination treatments and in vitro fertilization, but are usually not interested in having diagnostic surgery.
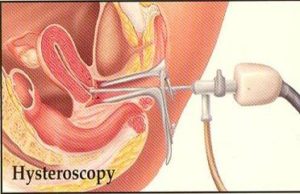
A hysteroscopy is a way for your doctor to look at the lining of your uterus. He or she uses a thin viewing tool called a hysteroscope. The tip of the hysteroscope is put into your vagina and gently moved through the cervix into the uterus. The hysteroscope has a light and camera hooked to it so your doctor can see the lining (endometrium) on a video screen.
A hysteroscopy may be done to find the cause of abnormal bleeding or bleeding that occurs after a woman has passed menopause. It also may be done to see if a problem in your uterus is preventing you from becoming pregnant (infertility). A hysteroscopy can be used to remove growths in the uterus, such as fibroids or polyps.
Your doctor may take a small sample of tissue (biopsy). The sample is looked at under a microscope for problems. Another surgery, called a laparoscopy, may also be done at the same time as a hysteroscopy if infertility is a problem.
» Find the cause of severe cramping or abnormal bleeding. Your doctor can pass heated tools through the hysteroscope to stop the bleeding.
» See whether a problem in the shape or size of the uterus or if scar tissue in the uterus is the cause of infertility.
» Look at the uterine openings to the fallopian tubes. If the tubes are blocked, your doctor may be able to open the tubes with special tools passed through the hysteroscope.
» Find the possible cause of repeated miscarriages. Other tests may also be done.
» Find and reposition a misplaced intrauterine device (IUD).
» Find and remove small fibroids or polyps.
» Check for endometrial cancer.
» Use heated tools to remove problem areas in the lining of the uterus (endometrial ablation).
» Place a contraceptive implant (Essure) into the opening of the fallopian tubes as a method of permanent sterilization.
